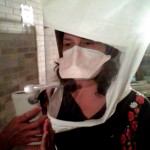
It happens every summer at hospitals and clinics across the country first-year and advanced residents and fellows start a new training-at-work year. As part of the infection control strategies at these healthcare facilities, respiratory protection training and fit testing campaigns move into full gear to ensure that everyone is covered (literally and figuratively). It is almost like the return of migrating birds as second, third and fourth-year residents and current fellows flock into queues for respirator use training, fit testing and, often, medical clearance for respirator use.
Providing these invaluable respirator program services en masse is a challenge for the infectious disease and industrial hygiene and EHS departments at hospitals and other healthcare facilities. Nationwide, according to the National Resident Matching Program (NRMP), more than 25,000 residents and fellows will begin their new assignments in July! Without interfering with patient care or hospital services, they all must be medically cleared, trained and fit tested for the sites selected respiratory equipment (sometimes 2 or 3 different manufacturers or styles) prior to stepping foot on the hospital floor. If you add nursing and other healthcare staff requiring an annual fit test in June or July, within a 4-6 week mid-summer period respiratory protection program departments at large teaching hospitals must provide OSHA-mandated support to 800 to 1000 (or more!) residents and fellows. Planning is imperative and cooperation from the medical staff makes the process smoother for everyone.
Do You Fit this Fit Test Profile?
In a recent campaign processing hundreds of medical staff, Emilcott provided support to the infectious disease and EHS fit testing teams at a regional teaching hospital. The fit test campaign coordinators orchestrated this event with military precision. It was well- planned and appropriately staffed. However, with so many folks donning respirators and fit test hoods, the lines were long and we encountered an array of challenging and uneducated attitudes. Here are some of our favorite responses:
- Im a third-year resident, I dont have to be clean shaven to get fit tested. (He was promptly handed a shaving kit.)
- What do you mean I failed? Is this graded? Oh, I see, the respirator failed, not me!
- I never wear those respirators, so can you make it quick.
- I know how to wear that. (As the respirator was put on upside down )
- I dont think I can work with this [fit test] hood on every day!
And, some real doozies during the 7-step qualitative fit test exercises:
- Just tell me, what is the right answer! Should I taste the Bitrex® or not? (We sent this doctor to be quantitatively fit tested.)
- Isnt this a bit excessive? Followed by Oh, now I think I can taste it!
- Cant you use that sweet stuff? I like that better than this bitter taste.
- This respirator fit okay last year why can I taste the bitter flavor now?
- This process didnt take this long at the last hospital I worked, you must be doing it wrong.
- And, drum roll please, from an Infectious Disease Fellow, Thank you for making us go through each step of the fit test procedure, its really important!
As a Certified Industrial Hygienist, my challenge is to convey the why, how and when of respirator use (according to OSHA Respirator Standard training and fit testing requirements) to anyone on my watch even when my target audience consists of impatient, high achieving and time-pressed medical professionals. In an odd role reversal, Im doing the life saving using occupational health and safety standards to protect their bodies as they do their jobs.
When Are Healthcare Providers Required to Use Respirators?
The Centers for Disease Control and Prevention (CDC) indicates the use of respirators for protection from infectious respiratory aerosols specifically those from patients with active tuberculosis and influenza.
- The CDC TB Elimination: Respiratory Protection in Health-Care Settings Fact Sheet specifies that particulate filter respirators certified by National Institute for Occupational Safety and Health (NIOSH) be used for protection against airborne M. tuberculosis including
- Non-powered respirators with N95, N99, N100, R95, R99, R100, P95, P99, and P100 filters (including disposable respirators); and
- Powered air-purifying respirators (PAPRs) with high-efficiency filters
- The Department of Health and Human Services Interim Guidance on Planning for the Use of Surgical Masks and Respirators in Health Care Settings during an Influenza Pandemic emphasizes that respirator use is a critical component of a system of infection control practices to prevent the spread of infection between infected and non-infected persons. Respirator use is indicated as follows
- N95 (or higher) respirators should be worn during medical activities that have a high likelihood of generating infectious respiratory aerosols, for which respirators (not surgical masks) offer the most appropriate protection for health care personnel.
- N95 respirators are also prudent for health care personnel during other direct patient care activities (e.g., examination, bathing, feeding) and for support staff who may have direct contact with pandemic influenza patients.
High Velocity Fit Testing
Another comprehensive qualitative fit test (QLFT) campaign at a large teaching hospital in New York City was scheduled across a broad span of times, crossing many days and weeks to accommodate the schedules of rounds, staff, patients and Human Resources. Emilcotts fit testing team became considerably more efficient this year by switching to the TSI Qfit to generate the test atmospheres. One touch of a button on these pump-driven nebulizers produces the equivalent of 5 bulb nebulizer compressions and uses quick, pop-on cartridges containing the challenge solutions. The easy and consistent delivery system of the nebulizers enabled us to focus our attention on the respirator user and the respirator fit.
Fit testing of course confirms (or not) the match of each face to the selected respirator. For respirator users who were unable to taste either Bitrex® or Saccharin during sensitivity testing; could not clear the taste of Bitrex® after wearing a poor fitting respirator; or, were extremely uncomfortable wearing the fit test hood, we supplemented the QLFT with quantitative fit testing (QNFT) to ensure an accurate respirator fit test. Staff that did not pass both the QLFT and QNFT with any standard-issue respirator was forwarded to the Respiratory Therapy department for personal respirator attention. In our estimation, more than 1000 staffers, new and seasoned, passed through our fit testing process in a matter of days!
Respiratory Protection is Smart
It is important for medical staff new or seasoned - to know when and why they are required to wear respiratory protection the training is an essential part of the OSHA Respirator Standard. While the attitudes we encounter during fit testing at hospitals often include dismay over a failure or impatience and ungraciousness, we do our best to educate each person as they roll through the lines. Many times, the mere mention of antibiotic-resistant TB exposure or gentle reassurance that a failed fit test is not the same as a failed biology test, can shift a nurse or doctors perspective. What was a nuisance can quickly turn into a better comprehension of their occupational risk and personal responsibility to protect their health. As for the others? As OSHA mandates, theres always next year.
As a health and safety professional, have you encountered any resistance to respirator fit testing? How have you responded? As a healthcare provider, what do you think about fit testing? Do you take it seriously? Does your employer?